-


A COMPARATIVE ANALYSIS OF DEMINERALISED FREEZE-DRIED BONE (DFDBA), FRESH FROZEN BONE ALLOGRAFT (FFBA) AND AUTOGENOUS BONE GRAFT (AU)—A HISTOLOGIC STUDY IN RABBITS
Objectives: There are different clinical applications for bone grafts in alveolar reconstructions and difficulties in achieving vertical osseous increase. This study was to make a comparative histological evaluation of DFDBA, FFBA, AU and blood clot (CO) on vertical guided bone regeneration (GBR) in rabbit calvaria. Methods: Nine rabbits were used. One was the primary bone graft donor and eight were GBR models, whereby 32 titanium cylinders were fixed to the calvaria and randomly filled with DFDBA, FFBA, AU or CO. The animals were killed 13 weeks later and the contents of the cylinders were analysed histomorphologically and histomorphometrically to quantify the total area (AT) of newly formed tissue, new bone (NB) and residual graft (RG) particles. Results: Mean values of AT were significantly higher for DFDBA and FFBA in the order DFDBA = FFBA > AU > CO. New bone formation with DFDBA and FFBA was better than with AU or CO. There were more RG particles in the DFDBA models, in the order FFBA > DFDBA = AU = CO (p values Conclusions: Allografts containing DFDBA and FFBA can be considered beneficial for achieving new vertical bone formation. -


STEM CELL BONE ALLOGRAFTS IN MAXILLARY SINUS AND RIDGE AUGMENTATION – REPORT OF A CASE
Objectives: To evaluate the use of an allograft cellular matrix containing live stem cells for maxillary sinus and ridge augmentations. Methods: Maxillary sinus and ridge augmentations were performed using an allograft cellular matrix containing live stem cells. The post-operative results were evaluated by CT scans and peri-apical radiographs. Sinus augmentation was evaluated after 10 weeks. Radiographic bone tomography was similar to that of the native bone and the ridge augmentation resulted in a vertical ridge augmentation of 3–4mm. The cellular matrix was supplied by Brockton, MA and processed by AlloSource, Centennial, CO. Results: Following healing and approximately 10 weeks following surgery, an additional CT scan was taken. This showed that the native and augmented bone was of an adequate width for supporting an implant. Radiography revealed that the augmented bone had a similar texture to native bone, indicating formation of mature bone. The scan also revealed downward growth of the bone in a vertical direction, overlapping the crest of the native pre-maxillary bone. This was not attempted during the surgical procedure, and was a particular cause for concern. Conclusions: This use of allograft mesenchymal stem cells has been shown to be a reliable method for ridge augmentation, especially in the vertical direction in areas of severe ridge atrophy. Further studies are needed to support this finding in a more guided manner, especially for vertical ridge augmentation. -

-

Cell-to-Cell Communication: Periodontal Regeneration
Stadlinger, Bernd / Terheyden, HendrikUnlike bone, which undergoes remodeling by resorption followed by bone apposition, teeth are not subject to physiological remodeling. They are remarkably resistant to physiological remodeling processes. The reason for this is found in the periodontium and cementum. The mechanisms that take effect in this area and the effectiveness of the periodontal system - consisting of gingiva, alveolar bone, periodontium and cementum - after injuries will be visualized in the new scientific 3D film, "Periodontal Regeneration".The visualization of these complex processes is of great interest for academic teaching as well as for the clinician and general practitioner as the cellular interactions are presented in the context of four phases. For the first time scanning electron microscopic images of real cells will be visualized allowing the comparison of their characteristics with computer animated simulations. DVD 1: Expert Version approx. 14 minutes DVD 2: Public Version approx. 13 minutes Outline: - Cementum formation - Orthodontic tooth movement - Trauma and periodontitis - Periodontal regeneration -

-
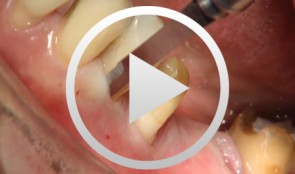

Periodontal Preserve Therapy (Examples)
Clotten, StefanContent: - Periodontal maintenance therapy for teeth 34 and 35, including the regeneration of a bone defect using bone replacement material, collagen membrane and sutures. - Curettage for treatment of periodontal pockets. - Treatment of gingival pressure sores caused by tight-fitting orthodontic apparatus. - Incision of buccal attachment to relieve gingival pressure for elimination of gingival recession. -
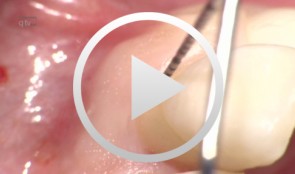

-

Treatment of a palatal class II furcation
Marggraf, ErwinOutline: - Reflecting a flap - Cleaning. - Fraction 3 - Fraction 2 - Fraction 1 - Wound closure List of materials All materials required for producing PRGF (BTI Germany) Bone replacement materials Geistlich Biomaterials Surgical instruments, Aesculap Suture materials, Ethicon -


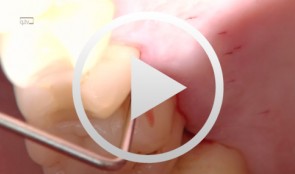
The use of autologous PRGF in periodontal plastic surgery
Marggraf, ErwinContents: - Blood sampling - Platelet separation activation - Introduction of bone replacement material - Access flap and curettage - Introduction of PRGF and bone replacement material - Plastic suture Materials Checklist: All materials required for producing PRGF (BTI Germany) Bone replacement materials Geistlich Biomaterials Surgical instruments, Aesculap Suture materials, Ethicon -
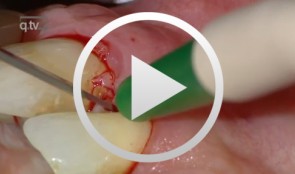

Periodontal regeneration at teeth 21 and 23 using EMD and cortical bone chips
Topoll, Heinz H.Contents: - Incisions using a microsurgical scalpel - Reflecting a buccal flap - Preparing papillary flaps using a microsurgical scalpel - Lifting off of the papillary flaps using a papillary elevator - Removing the granulation tissue using an ultrasound scaler - Cleaning the dental roots using manual instruments - Trying to dental root - Applying Emdogain - Mixing Bio-Oss and Emdogain - Introducing the Bio-Oss into both bone defects - Microsurgical suturing Materials Checklist: Cheek retractor Microsurgical scalpel blade holder Microsurgical scalpel blade Soniflex tips Bone rest Castroviejo microsurgical needle holder Suturing scissors Dental tweezers Microsurgical tweezers Monofilament suturing material 6/0 Seralene Pref gel Emdogain Bio-Oss